INTRODUCTION
Diabetic foot ulcer infection (DFI) represents a serious and often complex clinical scenario in modern day practice. DFI represents close to 10% of all hospital admission and reaching peaks of being the cause of one in every three orthopaedic admissions in general hospitals locally.
The equally important contributory factor of this occurrence is the fact that Malaysia has seen a surge of the prevalence of Diabetes mellitus with the latest number at 17.5% based on National Health and Morbidity Survey (NHMS) 2015 which was an increase of nearly 20% when compared to NHMS 2011.
As matter of fact, Malaysian population had seen the rate of obesity (a key pre-disposing factor to diabetes) peak to almost 1 in 2 Malaysian adults, hence propelling Malaysia into the limelight for having the highest amount of obese population in South East Asia according, to a report by the World Health Organization (WHO) on non-communicable diseases (NCD) in 2011.
Management of DFU demands a multi-team approach and often diagnosed at primary health centres and general practice. Complication of DFU in patients is usually due to:
- prolongation of poorly regulated blood glucose
- neuropathy which affects mainly sensory and proprioception
- reduced blood supply due to atherosclerosis
- decreased immunity due to macrophage capability
Causative organism in DFI is usually polymicrobial in nature which has a high prevalence of mixed organisms including S. Aureus, Streptococcus, E. coli, Klebsiella, Enterobacter, and P. aeruginosa.
One of the most dreaded complication of DFU is digit and limb amputation. Addressing all these risk factors can lower the incidence of lower limb amputations. Clinically, the main aim is to reduce organism load by classically wound debridement and in selected few mild infections with empirical antibiotics. Wound closure and wound care be a priority in addition to limiting recurrence.
In the light of the steep increase in DFU within the local clinical environment, there appears to be an increment in patient attention to mainly nonsurgical treatments, alternative medicine and the use of the supplements. This creates a problem for the general practitioner as there is a huge paucity of scientific information. Patients are often exposed to a variety of products on social media which has limited unbiased clinical trials done locally. Almost all treatments do not have USA Food Drug Agency (FDA) approval.
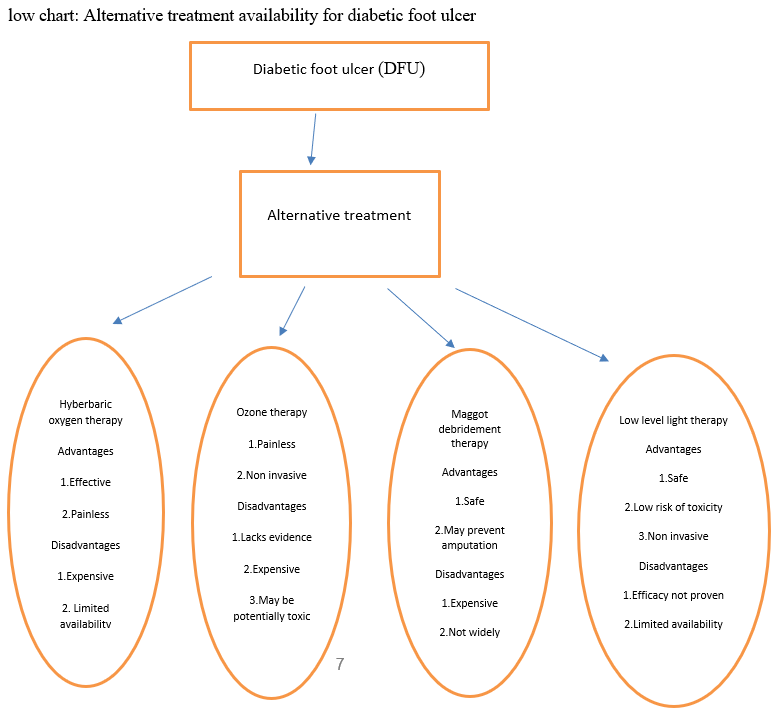
This review would serve as a short guide for primary care physician in dealing with patients who seek information about the efficacy, practicability, cost-benefit factor and especially the safety of these products and treatments which will cover newer technologies available locally like hyperbaric oxygen therapy, low-level light therapy, ozone therapy plus complementary alternative medicine (e.g. herbal products, essential oils, and miracle health products made famous on social/mass media platform).
- Newer Technologies in Alternative Medicine
- Hyperbaric Oxygen Therapy (HBOT)
HBOT is rapidly gaining popularity as an effective adjuvant therapy by enhancing wound epithelisation and fastening the process of wound closure. DFU post-wound debridement is usually a large wound that would require daily dressing. The granulation tissue over the bear structure including muscle, tendon and occasionally exposed bone is dependent on multiple factors. Exposure to HBOT would increase local concentrations of oxygen, fibroblast formation, and improve epithelisation rate. Undersea & Hyperbaric Medical Society (UHMS) defines HBOT as a treatment in which a patient intermittently breathes 100% oxygen while the treatment chamber is pressurised to an atmospheric pressure greater than sea level. The pressure increase must be systemic through the use of mono- or multiple chambers.
Since 1967, HBOT has been reported to enhance oxygenation, fibroblast proliferation, collagen synthesis, epithelialisation and neovascularisation, increased bactericidal activity, and is toxic to anaerobes (Hunt TK., 1988). Zamboni et al., 1997 found a significantly greater reduction in wound size with HBOT in a small, non-randomised study, though the control group consisted of only five patients who refused HBOT therapy. Abidia et al., 2003 conducted a double-blind randomised controlled trial which demonstrated improved healing and cost-benefits with adjunctive HBOT in diabetic ulcers, compared to a placebo group receiving only hyperbaric air, although the sample size was once again small. Another recent study by Kessler et al., 2003 found a doubling of the mean healing rate of non-ischaemic chronic foot ulcers in selected diabetic patients treated with HBOT.
Malaysian Armed Forces Health Services (MAFHS) has been pioneering this newer method of technology at Terendak Hospital since 1996 with great efficiency and good safe track record. This method has gained so much popularity that it has been offered to government patients in more than four locations and at least five newer centres in the private sector with abundant choices in Klang Valley.
In summary, HBOT is a relatively safe, non-invasive means of improving healing by enhancing the oxygenation, decreasing edema, and modifying the healing and immune responses against the wound. Cases that would benefit from this type of adjuvant therapy are DFU in well-controlled diabetes and post wound debrided wounds. Limb preservation and a faster healing time make this a cost-effective method of wound care. However, the protocols of treatment regime vary greatly. Hence, further research is needed to establish its efficacy and safety of use in Malaysia.
- Maggot Debridement Therapy (MDT)
Maggot therapy has seen a recent rise in its use in local hospitals and specialised centres in the management of chronic DFU.The most used species of maggots that is the Lucillia species Phaenicia Sericata larvae/maggots, which are able to survive by feeding exclusively on dead, necrotic tissue plus excessive slough. Its unique ability to only feed on unwanted tissue makes it a safe and relatively cheap option in enhancing wound closure.
Medical maggots secrete a digestive enzyme that selectively dissolves necrotic tissue, disinfects the wound and stimulates wound healing. These helpful enzymes include carboxypeptidases A and B, leucine aminopeptidase, collagenase, and serine proteases (trypsin-like and chymotrypsin-like enzymes).
Numerous large cohorts and recent retrospective reports show significantly greater wound healing rates when compared against conventional therapy. Similarly, a recent meta-analysis by Wilasrusmee C, et al 2013 of more than 35 retrospective studies done previously, showed MDT is significantly better for wound healing and more cost-effective than conventional therapy. The study outlines MDT therapy showed an improved healing rate of 15.99 days and costing on the average 40% less when compared to conventional therapy. Nevertheless, MDT does pose side effects like isolated cases of pain, malodour, and stigmata of using larvae. Overall, MDT is a safe viable option alternative to surgical debridement, decreases time to healing and stay of patients in the ward, which may decrease the risk of major amputations in selected DFU patients.
- Ozone Therapy
Another well-known alternative management making a buzz among the public is ozone therapy. There are various techniques for ozone therapy, including autohemotherapy (also known as autologous blood transfusion), direct intra-arterial and intravenous injections, rectal insufflations, intramuscular injection, ozonised water, intra-articular injection, ozone bagging and the use of ozonised oil. Ozone therapy requires administration of precise therapeutic levels to make sure that the treatment works. Otherwise, the treatment will fail if the dose provided is too low or alternatively toxic if the dose prescribed is too high. Although ozone therapy has its drawbacks, some researchers believed that it has many therapeutic effects.
After the turn of the century, there has been a surge of interest among diabetic patient in the use of ozone therapy. Ozone therapy has spread to the shores of Malaysia especially in the beauty and wellness sector. Although there many routes of administration of high level of Oxygen to the body but autohemotherapy or also known as autologous blood transfusion appears to be the preferred method of administration. Other methods of delivery would include direct intra-arterial and intravenous injections, intramuscular injection, ozonised water, intra-articular injection, ozone bagging and the use of ozonised oil.
The actual regimes and modes of administration including the addition of intravenous antibiotics seem to lack consistency and evidence. Health Technology Assessment Section, Ministry of Health (MaHTAS), published an updated report in 2017 regarding the safety of this therapy. The objective was to assess the safety and efficacy of autohemotherapy. MaHTAS reported no new high-level evidences.
There was very limited evidence, if any, on its use for treatment of chronic limb ischemia which was also limited by the problem of small sample size, no binding or use of placebo therapy. In terms of safety, it has been reported as exposing patients to the risk of blood-borne diseases such as ever increasing incidences of the transmission of hepatitis infection as. In conclusion, more high-quality evidence is needed.
- Low-Level Light Therapy (LLLT)
Low-level light therapy (LLLT) or commonly known as phototherapy has gained popularity in certain regions of the world including Malaysia. LLLT was developed by Andre Mester in the late 1960s and has been used extensively by the aesthetics and wound care industry. The basic concept of LLLT treatment resides in the absorption of light by photo acceptors or chromophores at the molecular, cellular, and tissue levels, that results in cellular changes including synthesis of collagen and extracellular matrix, recruitment of cytokines and growth factors, migration, proliferation, and differentiation of cells. LLLT achieved more rapid wound epithelialisation and wound closure in post wound debrided DFU patients.
There are few systematic review studies of randomised controlled trials which suggested that when compared to no therapy or placebo, LLLT may increase the healing rates of DFUs wounds during follow-up and may reduce wound size. However, most studies are conducted with small sample size or methodological flaws. Hence, the quality of this evidence is relatively low. Large, well-designed randomised controlled trials are needed to confirm whether LLLT could be an effective option. As for 2018, there seems to be a paucity of validated evidence regarding clinical efficacy and the use in DFU patients.
- Pharmacological care
- Antibiotics and Dressings
It is important to ensure the correct antibiotic is being used which will indirectly help to prevent any antimicrobial resistance (AMR) from emerging. The decision to start the antibiotic regime, dosage form whether topical, oral or intravenous and duration all depends on the wound severity and treatment prognosis. Commonly used oral antibiotics include oral Amoxicillin & Clavulanic Acid 625mg TDS or oral Ampicillin & Sulbactam 375mg BD for 1 to 2 weeks in mild cases.
In severe cases, Intravenous Ampicillin & Sulbactam 1.5g-3g or Intravenous Ceftriaxone 1g-2g OD. As diminished sweating is a commonly associated condition, topical moisturising creams such as aqueous cream is also indicated if the surrounding skin of the wound is dry and cracked.
Treatment care plan of DFUs will depend on the clinical severity that ranges from mild to severe. Nonsevere cases may not require pharmacological treatment of antibiotics. Instead, wound care with meticulous dressings and assisted debridement of the wounds is adequate most of the time.
When dealing with DFUs, hydrogels are more efficacious than basic wound contact dressings, and non-adherent dressings are more cost-effective than Hydrofiber dressings. Ultimately, dressing choice should be tailored to the wound and the patient.
Products such as Profore 18-25cm, Prontosan® Wound Irrigation solution (350mL), Prontosan® Wound Gel (30mL), Dermacyn® wound care solution (500mL), Dermacyn® wound care hydrogel (50g), DuoDerm®, Kaltostat® 7.5 x 12.0 cm, Bactigras® 15 x 20cm, Stimulen Gel®, Stimulen Lotion®, Gold Dust®, and RTD Wound Dressing® are often available over the counter in pharmacies for outpatients. These products are registered and have reliable efficacy and safety profile. They will only be recommended by the pharmacist based on the type and severity grade of the DFUs upon inspection.
- Complementary & Alternative Medicine (CAM)
The main concern regarding the use of CAM is when patients visit dubious herbal shops (Toko Jammu) or untrustworthy medical e-shopping portals / social media pages in search of a miracle health product(s). Some of these websites may recommend unreliable wound care products which may claim to contain essential oils from roots such as Aquilaria Malaccensis (Agarwood) to promote wound healing or dubious supplements which may claim to contain plant ingredient such as Clinacanthus Nutans (Belalai Gajah) for patients with underlying chronic medical conditions.
These products, which at times are openly sold in night markets, are mainly brought in illegally from neighbouring countries or even prepared and packaged at home. Although these products are derived from herbal ingredients, they need to be in the pharmaceutical dosage form and to be registered with the National Pharmaceutical Regulatory Agency (NPRA).
There are vast pharmacodynamics technicalities involved when dealing with pharmacognosy, which is defined as the branch of knowledge concerned with medicinal drugs obtained from natural sources such as plants. Hence, unregistered products are generally unsafe and of unproven efficacy. The content may be adulterated with scheduled poisons such as steroids to “improve effectiveness”. The manufacturing, methods may also not adhere to good manufacturing practice. Although the enforcement team is continuously cracking down on the sale of unregistered products, however, due to a lack of knowledge and pure desperation for the cure of serious health problem, there is still a massive demand for these products.
In term of food supplements such as apple cider vinegar, cranberry juice or wine, the evidence is still equivocal regarding its’ effectiveness. Furthermore, the easy availability on online/e-shopping websites along with aggressive advertising on social media regarding food supplements in DFU treatment, masks the fact that there are almost no solid clinical evidence regarding its efficacy.
- Role of Community Pharmacist(CP)
It is vital for general practitioners to advise outpatients to purchase wound care products or any supplements for their underlying medical condition from a registered community pharmacist (CP). In Malaysia, CPs are bound by laws such as the Poison Act 1952 and Sale of Drug Act 1952, which are enforced by the Pharmaceutical Services Division. The enforcement team will frequently audit CPs to ensure that they comply with the rules and legislation pertaining to their license and sale of registered products.
Indirectly, this ensures that health products sold are of quality, safe, efficacious and suitable for the Malaysian population. CPs are also bound to professional regulations such as the Community Pharmacist Benchmarking Guideline. Along with CPs, they are also the most reliable source to purchase any health products as they adhere to Good Pharmacy Practice and Good Dispensing Practice.
CONCLUSION
The newer emerging modalities of treatment for DFU have gained popularity, especially with aggressive online advertising and social media effect on patient expectations. Hyperbaric Oxygen Therapy and maggot debridement therapy are evolving methods of treatment diabetic foot ulcer which demonstrated sufficient clinical evidence and serves a good adjuvant in wound care management especially after proper wound debridement. LLLT, complementary medicine, supplement, and traditional medicine have a very limited role to play in modern practice. These practices lack evidence plus possess a huge strain in total cost of treatment. Concomitant optimization of ischemia, infection, general patient well-being, wound management and adequate offloading of the foot remains the mainstay of treatment of Diabetic foot ulcer.
REFERENCES:
- Abidia A et al. The role of hyperbaric oxygen therapy in ischaemic diabetic lower extremity ulcers: a double-blind randomized-controlled trial. Eur J VascEndovasc Surg. 2003 Jun;25(6):513-8.
- Bakker DJ. Hyperbaric oxygen therapy and diabetic foot. Diabetes Metab Res Rev 2000; 16(Suppl. 1): S55–8.
- Clinical Practice Guidelines: Management of Diabetic Foot, Ministry of Health, Malaysia 1st Edition 2004.
4.Clinical Practice Guidelines: Management of Type 2 Diabetes Mellitus, Ministry of Health, Malaysia 5th Edition 2016
- Institute For Public Health Malaysia. National Health and Morbidity Survey 2011 (NHMS 2011). Non-Communicable Diseases.
- Institute For Public Health Malaysia. National Health and Morbidity Survey 2015 (NHMS 2015). Non-Communicable Diseases.
- Kessler L et al. Hyperbaric oxygenation accelerates the healing rate of nonischemic chronic diabetic foot ulcers: a prospective randomized study. Diabetes Care. 2003 Aug;26(8):2378-82.
- Peter Gál, Martin Bjørn Stausholm, Ivan Kováč, Erik Dosedla, Ján Luczy, František Sabol and Jan Magnus Bjordal, Should open excisions and sutured incisions be treated differently? A review and meta-analysis of animal wound models following low-level laser therapy, Lasers in Medical Science, (2018)
- Ronald A. Sherman. Maggot Therapy for Treating Diabetic Foot Ulcers Unresponsive to Conventional Therapy; Diabetic Care, volume 26, number 2, February 2003
- Zamboni WA, Wong HP, Stephenson LL, Pfeifer MA. Evaluation of hyperbaric oxygen for diabetic wounds: a prospective study.Undersea Hyperb Med 1997; 24:175-9.
- Wilasrusmee C, Marjareonrungrung M, Eamkong S, Attia J, Poprom N, Jirasisrithum S, Thakkinstian A. Maggot therapy for chronic ulcer: a retrospective cohort and a meta-analysis. Asian Journal of Surgery 2014; 37(3): 138-147
A clinician’s guide to newer alternative methods of treatment for general practitioners
Dr Navin Kumar A/L Devaraj
Family Medicine Specialist
Department of Family Medicine
Faculty of Medicine and Health Sciences
Universiti Putra Malaysia
MMA Member, Selangor
knavin@upm.edu.my
Dr Sanjiv Rampal Lekhraj Rampal
Orthopaedic Surgeon
Department of Orthopaedics
Faculty of Medicine and Health Sciences
Universiti Putra Malaysia,
Life Member Wilayah MMA
rampalsurgery@gmail.com
Dr Yeap Ewe Juan,
Consultant Orthopaedic Surgeon,
Prince Court Medical Centre
Tarikh Input: 29/05/2019 | Kemaskini: 15/02/2023 | h_khairi
PERKONGSIAN MEDIA










.png)
.png)
.png)














